Melasma Skin Condition Overview
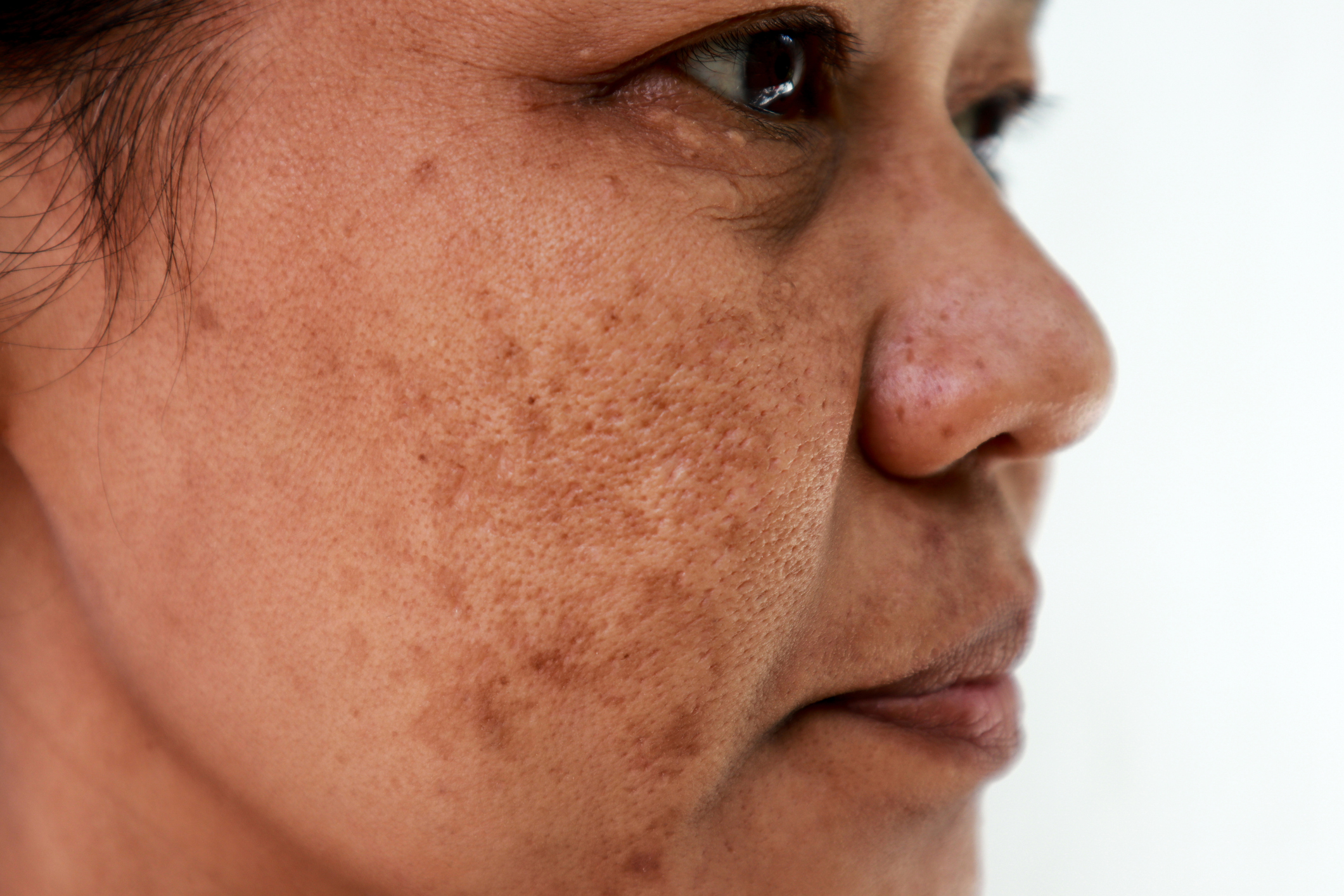
Melasma is a common skin condition that causes brown, gray-brown, or blue-gray patches or spots, typically on the face. It’s a form of hyperpigmentation due to overproduction of melanin (the pigment that gives skin its color). It’s often called the “mask of pregnancy” or chloasma because it frequently appears during pregnancy. It is triggered by sun exposure, hormones (pregnancy, birth control), genetics, and sometimes visible light or heat. There is no cure, but it can be effectively managed and faded with consistent treatment. Results take time (weeks to months), and maintenance is essential to prevent recurrence.
What It Looks Like
Melasma appears as flat, irregular brown or gray-brown patches with well-defined borders. Common locations include:
- Cheeks
- Forehead
- Bridge of the nose
- Upper lip (sometimes called a “melasma mustache”)
- Chin and jawline
It is usually symmetrical (affecting both sides of the face) and becomes more noticeable with sun exposure. It can also rarely appear on other sun-exposed areas like the forearms or neck.
Who Gets Melasma?
- Primarily women (about 90% of cases), especially those aged 20–40.
- More common in people with medium to darker skin tones (e.g., Hispanic, Asian, African, or Middle Eastern descent) who tan easily.
- Affects 1.5–33% of the population depending on the group, and up to 50% of pregnant women.
Men can get it too, but it’s less common.
Causes and Triggers
The exact cause isn’t fully understood, but it involves overactive melanocytes (pigment cells). Key factors include:
- Hormones — Pregnancy, birth control pills, hormone replacement therapy.
- Sun exposure — UV light, visible light, and heat are major triggers and worsen it.
- Genetics — Family history increases risk.
- Other contributors — Certain medications, skincare products that irritate the skin, thyroid issues, or stress.
Is It Harmful?
Melasma is harmless and not contagious or cancerous. However, it can cause emotional distress due to its appearance.
Treatment Options
Melasma is chronic and can relapse, so treatment focuses on control rather than a permanent cure. Results take time (often months) and consistency is key. Always consult a dermatologist for personalized advice.
1. Sun Protection (Essential Foundation for All Treatments)
Strict photoprotection is the most important step—melasma often worsens without it.
- Use a broad-spectrum sunscreen with SPF 30–50+ daily (reapply every 2 hours outdoors).
- Prefer mineral sunscreens (zinc oxide/titanium dioxide) with iron oxides (tinted formulas) for protection against UV + visible light/HEV (blue light from screens/indoors), which can trigger melasma.
- Wear wide-brimmed hats, seek shade, and avoid peak sun hours. Minimize hormone triggers (e.g., certain birth control) if possible.
2. Topical Treatments (First-Line Options)
These are applied directly to the skin, often at night.
- Triple combination cream (e.g., Tri-Luma: 4% hydroquinone + 0.05% tretinoin + 0.01% fluocinolone): The gold-standard, FDA-approved option. It lightens pigment, promotes cell turnover, and reduces inflammation. Use for short periods (up to 8–12 weeks) under supervision due to potential irritation.
- Hydroquinone (2–4%): A potent lightening agent (tyrosinase inhibitor). Often combined with tretinoin and a mild steroid. Available by prescription; not for long-term continuous use.
- Alternatives/Gentler Options (especially for sensitive skin, pregnancy, or hydroquinone concerns):
- Azelaic acid (15–20%): Anti-inflammatory and lightening; safe in pregnancy.
Tranexamic acid (topical). - Kojic acid, niacinamide, cysteamine, vitamin C.
- Retinoids (tretinoin/retinol): Increase cell turnover.
Dermatologists often recommend starting with these and monitoring for irritation.
3. Oral Medications
- Tranexamic acid (oral): Effective for moderate-to-severe or stubborn melasma. It reduces pigment production and blood vessel involvement. Used as an add-on under medical supervision.
4. Procedural Treatments (For Resistant Cases)
These are often combined with topicals for better results and are performed by professionals.
- Chemical peels (e.g., glycolic acid, salicylic acid): Exfoliate surface pigment. Multiple sessions may be needed.
- Microneedling: Can enhance topical absorption; sometimes combined with PRP.
- Lasers/Light Therapies (e.g., low-fluence Q-switched, fractional, IPL, picosecond): Target pigment but carry risks like worsening pigmentation (especially in darker skin tones). Reserved for refractory cases; results can be temporary.
- Other emerging options: Certain hybrid peels or advanced light devices.
Note: Procedures work best as adjuncts and require experienced providers to minimize side effects like post-inflammatory hyperpigmentation.
General Treatment Approach
- Mild cases: Sun protection + topical agents (e.g., azelaic acid or hydroquinone combo).
- Moderate/Severe: Triple combo + oral tranexamic acid if needed + procedures.
- Maintenance: Continue gentle topicals, strict sun protection, and periodic touch-ups.
- Expect gradual improvement; full results can take 3–6+ months. Melasma may recur with triggers.
Consult a professional for personalized advice, especially to rule out other conditions, assess skin type (darker tones need extra caution with lasers/hydroquinone), and monitor for side effects. Pregnant individuals should use pregnancy-safe options like azelaic acid.
Lifestyle tips: Avoid irritating products, scented soaps, excessive screen time (if a trigger), and waxing on affected areas. Consistent adherence yields the best outcomes.
Avoid irritants and over-the-counter “miracle” products that can inflame skin and darken patches.
Prevention and Management Tips
- Daily sunscreen and sun avoidance year-round.
- Gentle skincare routine (avoid harsh scrubs or products with alcohol/fragrance).
- If pregnant or on hormones, discuss with your doctor.
- Be patient—improvement is gradual, and maintenance therapy is often needed.
If you have melasma or think you might, see a professional for accurate diagnosis (it can resemble other conditions) and tailored treatment. Outcomes are best with professional guidance.